A practical clinical reference for managing type 2 diabetes in the outpatient setting — covering the 2024 ADA/EASD consensus on glycaemic targets, drug sequencing, and the monitoring schedule that keeps complications at bay.
The 2024 ADA/EASD Consensus: Patient-Centred Care
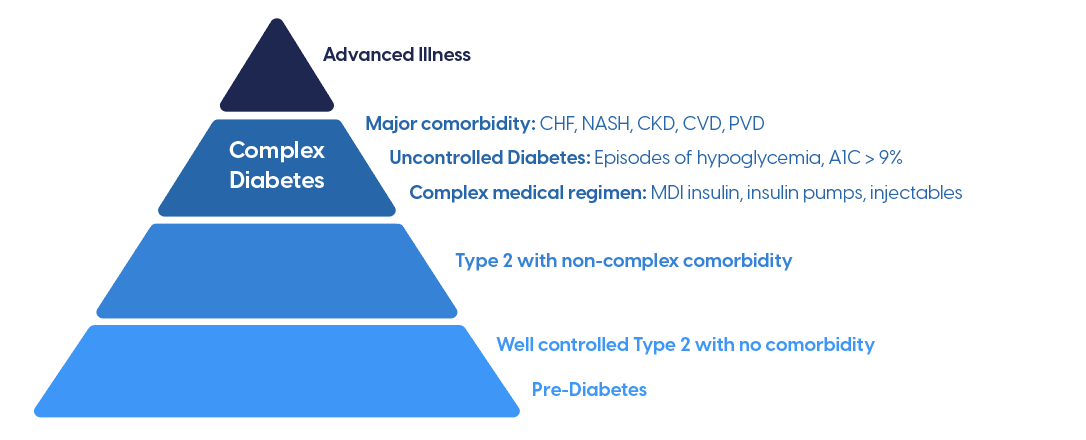
The 2024 joint ADA/EASD consensus update emphasised individualisation of glycaemic targets rather than a universal HbA1c goal. The appropriate target depends on:
- Duration of diabetes and life expectancy.
- Presence of established CVD, CKD, or heart failure.
- Hypoglycaemia awareness and risk.
- Patient preference and socioeconomic factors.
Glycaemic Targets
| Patient Profile |
HbA1c Target | --- |
--- | Newly diagnosed, low comorbidity |
< 6.5% | Most adults with T2DM |
< 7.0% | Established CVD or CKD |
< 7.0–7.5% | Frail elderly, limited life expectancy |
< 8.0–8.5% | Pregnancy (pre-existing T2DM) |
< 6.5% |
Drug Sequencing
Metformin remains the preferred initial agent in the absence of contraindications (eGFR < 30 is a contraindication; use with caution at eGFR 30–45).
However, if the patient has established atherosclerotic CVD, heart failure, or CKD at diagnosis, the 2024 consensus recommends initiating an
SGLT-2 inhibitor and/or
GLP-1 receptor agonist alongside or instead of metformin, because of their proven cardiovascular and renal benefits beyond glycaemic control.
Second-Line Addition
- SGLT-2 inhibitor: empagliflozin, dapagliflozin, canagliflozin — favoured in heart failure and CKD.
- GLP-1 RA: semaglutide, liraglutide, dulaglutide — favoured in established CVD and in patients needing significant weight reduction.
- DPP-4 inhibitor: saxagliptin, sitagliptin — weight-neutral, well tolerated, but no CV benefit (saxagliptin associated with HF hospitalisation — avoid in HF).
- Sulfonylurea: low cost, effective, but hypoglycaemia risk and weight gain limit use.
Monitoring Schedule
At Every Visit
- Foot inspection (10-g monofilament for neuropathy screening annually).
- Medication adherence and tolerance.
Every 3 Months
- HbA1c (until at target, then every 6 months).
- Fasting glucose review if on insulin.
Annually
- Urine ACR and eGFR (renal function).
- Dilated fundus examination (diabetic retinopathy screening).
- ECG if cardiovascular risk is high.
Hypoglycaemia Recognition & Management
Hypoglycaemia (< 70 mg/dL) is a medical emergency risk in patients on insulin or sulfonylureas. Educate patients on the rule of 15: 15 g of fast-acting carbohydrate, recheck in 15 minutes. For severe hypoglycaemia: 1 mg glucagon IM or SC (or intranasal), call emergency services.
Documenting Diabetes in ClinIT
ClinIT's structured chronic-disease note template includes HbA1c trend charts, medication titration history, foot exam findings, and annual review checklist. Automated flags alert the doctor when a patient's annual renal or eye check is overdue.