Manual IOL calculations carry unnecessary risk. Clinit embeds five biometry formulae directly into the pre-op workflow — here's why that matters for patient safety.
The Stakes of IOL Calculation
Intraocular lens power selection is one of the highest-stakes decisions in elective surgery. A one-dioptre error in a 55-year-old bilateral cataract patient means years of spectacle dependence after a procedure they chose to avoid exactly that outcome.
Clinit's IOL calculator supports:
- SRK/T — workhorse for average axial length
- Holladay 2 — complex eyes
- Haigis — steep/flat corneas, post-LASIK
- Barrett Universal II — modern benchmark
- Kane — AI-enhanced, best overall performance
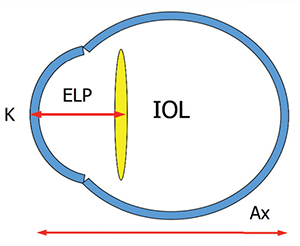
Biometry inputs (AL, K1, K2, ACD, LT, CCT) are entered once; all five formulae compute simultaneously. The surgeon sees a comparison table and selects the target power and planned post-op refraction in the same screen.
Pre-op to Post-op Continuity
The selected IOL power is carried into the operative note, the discharge summary, and the 1-week and 6-week follow-up templates. No re-entry means no transcription errors.
Myopia Management Module
Beyond cataract, the optical module tracks axial length progression in paediatric myopia patients, overlays the child's trajectory against population percentiles, and flags accelerating progression for intervention review.
Refraction History Timeline
Every refraction entered into Clinit is plotted on an SE (spherical equivalent) trend chart. Patients and referring GPs can view the trend via the patient portal.